BIGBEAR
PHARMACEUTICAL
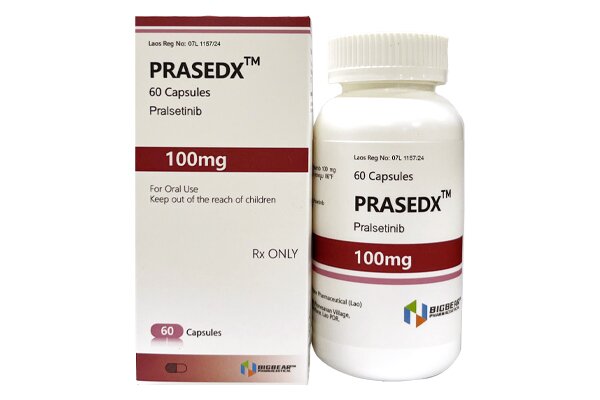
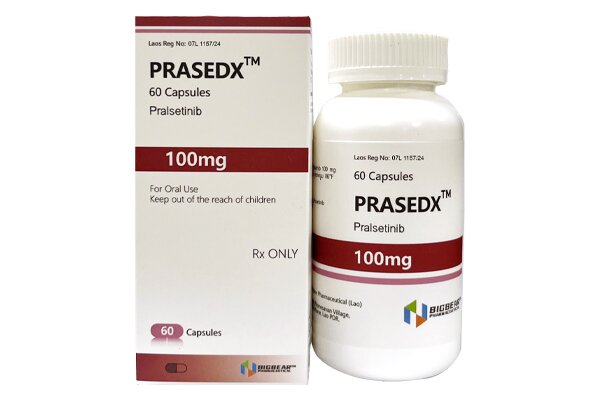
Pralsetinib inhibits the abnormal activation of RET protein and blocks downstream signaling pathways.

 Authentic
Authentic Guarantee
Guarantee Fast Delivery
Fast Delivery Privacy
Privacy Pralsetinib is an oral small-molecule tyrosine kinase inhibitor (TKI) that selectively targets RET (Rearranged during Transfection) gene fusions and mutations. It is indicated for adult patients with metastatic non-small cell lung cancer (NSCLC) confirmed to be RET fusion-positive by an FDA-approved test, as well as pediatric patients aged 12 years and older and adult patients with RET fusion-positive advanced or metastatic thyroid cancer who require systemic therapy and are radioiodine-refractory (if radioiodine is applicable).
1.This product is indicated for the treatment of adult patients with locally advanced or metastatic non-small cell lung cancer (NSCLC) who harbor a rearranged during transfection (RET) gene fusion.
2.This product is indicated for the treatment of adult and pediatric patients aged 12 years and older with advanced or metastatic RET-mutant medullary thyroid cancer (MTC) requiring systemic therapy, as well as adult and pediatric patients aged 12 years and older with advanced or metastatic RET fusion-positive thyroid cancer requiring systemic therapy and who are radioiodine-refractory (if radioiodine is applicable).
This indication is approved conditionally based on the results of a study in RET-mutant MTC and RET fusion-positive thyroid cancer. Full approval of this indication is contingent upon the clinical benefit demonstrated in ongoing confirmatory trials.
This product should be prescribed by a physician experienced in anti-tumor therapy.
Prior to initiating treatment, it must be confirmed that the patient has a RET gene fusion (for non-small cell lung cancer or thyroid cancer) or mutation (for medullary thyroid cancer) detected by a fully validated testing method.
The recommended dose is 400 mg orally once daily, on an empty stomach (at least 2 hours before and 1 hour after eating). Treatment should continue until disease progression or unacceptable toxicity occurs.
If a dose is missed, take it as soon as possible on the same day, and resume the regular daily dosing schedule the next day.
If vomiting occurs after taking a dose, do not take an additional dose; continue with the next scheduled dose as planned.
First reduction: 300 mg once daily.
Second reduction: 200 mg once daily.
Third reduction: 100 mg once daily.
Patients who cannot tolerate 100 mg once daily should permanently discontinue treatment.
Grade 1 or 2: Temporarily discontinue treatment until the adverse reaction resolves, then resume at a reduced dose (per the reduction levels above). If ILD/non-infectious pneumonitis recurs, permanently discontinue treatment.
Grade 3 or 4: Permanently discontinue treatment.
Grade 3: If hypertension remains Grade 3 after antihypertensive treatment, temporarily discontinue treatment. Once blood pressure is controlled to ≤ Grade 2, resume at a reduced dose.
Grade 4: Discontinue treatment.
Grade 3 or 4: Temporarily discontinue treatment and monitor aspartate aminotransferase (AST) and alanine aminotransferase (ALT) weekly until the adverse reaction resolves to Grade 1 or baseline. Resume at a reduced dose. If Grade ≥ 3 hepatotoxicity recurs, permanently discontinue treatment.
Grade 3 or 4: Temporarily discontinue treatment until bleeding resolves to Grade 0/1 or baseline. If a severe or life-threatening hemorrhage occurs, permanently discontinue treatment.
Grade 3 or 4: Temporarily discontinue treatment until the adverse reaction improves to ≤ Grade 2, then resume at a reduced dose. If Grade ≥ 4 adverse reactions recur, permanently discontinue treatment.
Note: Adverse reactions are graded per the National Cancer Institute Common Terminology Criteria for Adverse Events (NCI-CTCAE) version 4.03.
Avoid concomitant use with known P-gp and strong CYP3A inhibitors. If unavoidable, reduce the current dose as follows:
Current dose of 400 mg once daily → reduce to 200 mg once daily
Current dose of 300 mg once daily → reduce to 200 mg once daily
Current dose of 200 mg once daily → reduce to 100 mg once daily
After discontinuing the P-gp and strong CYP3A inhibitor for 3–5 half-lives, resume the dose that was used before initiating the inhibitor.
Avoid concomitant use with strong CYP3A inducers. If unavoidable, starting on day 7 of co-administration, increase the starting dose to twice the current dose.After discontinuing the inducer for at least 14 days, resume the dose that was used before initiating the inducer.
Based on animal study findings and the mechanism of action of this product, administration to pregnant females may cause fetal harm. There are no clinical data on the use of pralsetinib in pregnant women to assess drug-related risks.
In pregnant rats dosed during the period of organogenesis, pralsetinib caused malformations and embryo-fetal lethality at maternal exposure levels lower than those achieved with the recommended human dose of 400 mg once daily.This product is contraindicated in pregnant females.
There are no data on whether pralsetinib or its metabolites are excreted in human milk, or on their effects on breastfed infants or milk production.Because of the potential for serious adverse reactions in breastfed infants, breastfeeding is not recommended during treatment with pralsetinib and for 3 weeks after the last dose.
The safety and efficacy of pralsetinib have been established in pediatric patients aged 12 years and older with RET-mutant medullary thyroid cancer (MTC) and RET fusion-positive thyroid cancer.
A thorough, well-controlled study in adult patients, along with additional population pharmacokinetic data, supports the use of pralsetinib in pediatric patients aged 12 years and older. Population pharmacokinetic data indicate that age and body weight have no clinically meaningful effect on pralsetinib pharmacokinetics, and exposure is expected to be similar between adults and pediatric patients aged 12 years and older.Given the comparable disease course of RET-mutant MTC and RET fusion-positive thyroid cancer in adults and pediatric patients, adult data can be extrapolated to pediatric patients.
The safety and efficacy of pralsetinib have not been established in pediatric patients with RET fusion-positive non-small cell lung cancer (NSCLC), or in pediatric patients younger than 12 years of age with RET-mutant MTC or RET fusion-positive thyroid cancer.
In the ARROW study, which included 438 patients receiving the recommended dose of 400 mg once daily, 30% of patients were aged ≥ 65 years.No differences in pharmacokinetics (PK), safety, or efficacy were observed between elderly patients and younger patients.
No studies have been conducted in patients with moderate hepatic impairment (total bilirubin > 1.5–3.0 × ULN, AST any) or severe hepatic impairment (total bilirubin > 3.0 × ULN, AST any).For patients with mild hepatic impairment (total bilirubin ≤ ULN and AST > ULN, or total bilirubin > 1.0–1.5 × ULN and AST any), no dose adjustment is needed.The safety and efficacy of this product in patients with severe hepatic impairment have not been established, so use is not recommended.
The most common adverse reactions are constipation, hypertension, fatigue, musculoskeletal pain, and diarrhea.
These include decreased lymphocytes, decreased neutrophils, decreased hemoglobin, decreased phosphates, corrected decreased calcium, decreased sodium, increased AST, increased ALT, decreased platelets, and increased alkaline phosphatase.
14.2% of patients permanently discontinued treatment due to adverse reactions.
The most common adverse reactions leading to permanent discontinuation (≥1% incidence) were non-infectious pneumonitis (1.4%) and infectious pneumonitis (1.4%).
61.0% of patients required temporary treatment interruption due to adverse reactions.
The most common adverse reactions leading to interruption (≥2% incidence) were neutropenia, non-infectious pneumonitis, anemia, hypertension, infectious pneumonitis, decreased neutrophil count, diarrhea, increased AST, increased creatine kinase, pyrexia, fatigue, increased ALT, asthenia, thrombocytopenia, vomiting, decreased white blood cell count, urinary tract infection, and dyspnea.
36.1% of patients required dose reduction due to adverse reactions.
The most common adverse reactions leading to dose reduction (≥2% incidence) were neutropenia, anemia, non-infectious pneumonitis, decreased neutrophil count, hypertension, and increased creatine kinase.
None.
Severe, life-threatening, or fatal interstitial lung disease (ILD)/non-infectious pneumonitis can occur in patients receiving this product.
If patients develop respiratory symptoms suggestive of ILD/non-infectious pneumonitis (e.g., dyspnea, cough, fever), immediately discontinue treatment and seek medical attention. Perform diagnostic evaluations, including imaging and infectious workup.
For patients with confirmed Grade ≥3 ILD: Permanently discontinue treatment.
For patients with Grade 1–2 ILD: Discontinue treatment until ILD resolves completely, then resume at a reduced dose. If ILD recurs at any grade after resumption, permanently discontinue treatment.
The most common management for hypertension developing during treatment is antihypertensive medication.
Uncontrolled hypertension is a contraindication to initiating this product. All patients should have baseline blood pressure measured before starting treatment, and monitored every 1–2 weeks thereafter. Initiate or adjust antihypertensive therapy as clinically indicated.If hypertension remains Grade 3 despite treatment, temporarily discontinue this product. Once blood pressure is controlled to ≤ Grade 2, resume treatment at a reduced dose.
Before initiating treatment, perform baseline liver function tests to assess AST and ALT levels.During the first 3 months of treatment, monitor AST and ALT every 2 weeks, then monthly thereafter or as clinically indicated.If AST/ALT elevations ≥ Grade 3 occur, temporarily discontinue treatment and monitor AST and ALT weekly until values return to Grade 1 or baseline. Resume treatment at a reduced dose. If Grade ≥3 hepatotoxicity recurs, permanently discontinue treatment.
Severe, including fatal, hemorrhagic events can occur in patients receiving this product.
If a severe or life-threatening hemorrhage occurs, permanently discontinue treatment and seek immediate medical attention.
Patients with large tumor burden, rapidly growing tumors, renal impairment, or dehydration are at higher risk of TLS.
Before initiating treatment, assess the patient’s risk of TLS and evaluate the potential benefit versus risk of treatment. If treatment is initiated, consider prophylactic measures (e.g., adequate hydration) and monitor for signs/symptoms of TLS and renal function, with prompt intervention as clinically indicated.
Patients receiving drugs that inhibit vascular endothelial growth factor (VEGF) signaling pathways, including this product, may be at risk for impaired wound healing.
Discontinue this product at least 7 days before elective surgery and do not resume for at least 2 weeks after surgery, until the wound is fully healed. The safety of resuming treatment after resolution of wound healing complications has not been established.
Based on animal study findings and the mechanism of action, administration to pregnant females may cause fetal harm. Animal data show that maternal exposure levels lower than those achieved with the recommended human dose of 400 mg once daily can cause malformations and embryo-fetal lethality.
Before initiating treatment, confirm the pregnancy status of females of reproductive potential.
Advise pregnant females of the potential risk to the fetus. Recommend that females of reproductive potential use effective non-hormonal contraception during treatment and for 2 weeks after the last dose, as this product may render hormonal contraceptives ineffective.
Advise males with female partners of reproductive potential to use effective contraception during treatment and for 1 week after the last dose.
Histopathological findings in the reproductive systems of male and female rats, and a dedicated fertility study (in which rats of both sexes were dosed and mated), indicate that this product may impair fertility.
If any issues arise, please contact us immediately.
Email:laosbigbear@gmail.com

Take the medication as soon as you remember. However, if it is nearly time for your next scheduled dose, skip the missed one. Do not take a double dose to compensate.
Seek immediate emergency medical assistance or call the Poison Help hotline.
Adhere to your doctor’s instructions regarding any restrictions on food, drink, or daily activities.
Certain drugs should not be used concurrently, as they may alter the blood concentration of other medications you are taking. This can increase the risk of side effects or reduce the effectiveness of your treatment.
Inform your doctor about all medications you are currently using. Many drugs may interact with pralsetinib, particularly:
Antibiotics or antifungal medications
Antiviral drugs for HIV or hepatitis C
Other anticancer medicines
Specific cholesterol-lowering drugs
Antiseizure medications
This list is not exhaustive. Numerous other medications may influence pralsetinib, including prescription drugs, over-the-counter products, vitamins, and herbal supplements. Not all potential drug interactions are listed here.
Copyright2024@ BIGBEAR All right reserved Bigbear | Bigbear Pharmaceutical | Bigbear Laos



